What You Need to Know about Kidney Transplant: Eligibility, Requirements, Process, Living Donation and More
Summary
Kidney transplants are the most successful organ transplants, with a 90-95% success rate, and their numbers are increasing. Here we overview key issues of concern for patients and potential donors.
Kidney transplant, although not a cure for kidney disease, is considered the optimal treatment for helping most patients live longer and with a better quality of life. The number of lifesaving transplants across all age groups, ethnicities, blood types and diagnoses in the U.S. is increasing, thanks in part to organ allocation policy changes that have taken effect since 2014 aiming to increase access to lifesaving organs. Other contributors include concerted efforts from stakeholders including donor families, the Organ Procurement Transplant Network (OPTN) and other organizations, transplant centers, and government policy reforms intended to address troublesome disparities and inequities that exist in organ donation, transplantation and dialysis.
While the number of transplants is increasing, intensified focus on the topic has also led to growth in the waitlist as well. In 2021, more than 90,000 patients were waiting for kidneys in the U.S., and only 27%, or 24,670, received a transplant, according to the Health Resources & Services Administration (HRSA). Today, there are about 93,000 people on the kidney transplant waitlist, according to the United Network for Organ Sharing (UNOS; the non-profit organization serving as the nation’s transplant system, under contract with the federal government).
Below, we overview some common questions about kidney transplantation for patients with end-stage kidney disease (ESKD; also referred to as ESRD or end-stage renal disease) and for those considering donating the gift of life. If you have or are approaching ESKD, be sure and talk to your doctor to see if transplant is an option for you. If it’s not an option, home dialysis may be a solution that can help you live your best life.
Eligibility
Many people with late-stage chronic kidney disease (CKD) and kidney failure are eligible for a transplant. However, some conditions may make it more difficult to have the surgery, or make it too high risk. Talk to your transplant center about their eligibility requirements. Not all transplant programs have the same criteria, so if other transplant programs are accessible to you, you may consider talking to more than one. You can be listed by more than one program.
Waiting for a transplant is not like taking a number and waiting your turn. The waitlist is better described as a large pool of patients. When a deceased organ donor is identified, UNOS’ computer system generates a ranked list of transplant candidates who are suitable to receive each organ. UNOS matches individuals waiting for a lifesaving transplant with compatible donor organs. Note that only medical and logistical factors are used in organ matching. Personal or social characteristics such as celebrity status, income or insurance coverage play no role in the priority of who is allocated a kidney (read more about UNOS here).
Did You Know?
A misconception is that a kidney transplant acts as a cure for chronic kidney disease. Actually, it is more of a replacement. Transplant can significantly aid a patient’s overall condition, improve and extend life, and eliminate the need for dialysis, but may not be the right choice for everyone (source: Texas Kidney Institute).
Also see “Are You Kidneying Me? 8 Kidney Disease Myths and Facts.”
Organ transplants are most successful when preservation and transport time are short. The UNOS matching system considers the distance between donor and transplant hospitals. In general, local candidates get organ offers before those listed at more distant hospitals. The UNOS Organ Center helps place donated organs for transplantation 24 hours a day, 365 days a year.
To determine eligibility, you may also need to undergo screenings such as these:
- Blood and tissue types
- HIV and hepatitis
- Mammogram and PAP (women)
- Prostate exam (men)
- Lung X-ray
- Heart evaluation (echocardiogram, electrocardiogram)
- Colonoscopy
- Mental health
- Financial
- Caregiver support
If you’re wondering when you can start inquiring about a transplant, the National Kidney Foundation (NKF) advises that it is best to begin early in your disease course, before you need dialysis. That way, you might be able to get a preemptive kidney transplant (PKT), meaning getting your transplant before needing to start dialysis.
It can take time to find the right transplant center, complete the transplant evaluation, explore live kidney donor options and get on the deceased donor transplant list if needed. If you are not yet on dialysis and have an estimated glomerular filtration rate (eGFR) of 20 or less, you can already begin building “wait time” on the deceased donor transplant list.
Types of Kidney Donation
You can receive either a deceased donor transplant or a living donor transplant. UNOS manages the list of all the people across the U.S. waiting for a deceased organ transplant. The organization ensures that deceased donor organs are distributed fairly using a transparent system. For kidneys, this is a combination of blood-type and antibody matching, time with kidney failure, and a few other factors that give people priority on the list (including being a child or being a past live kidney donor). Although most deceased donor kidneys function immediately during surgery, some deceased donor kidneys do not, and as a result, the patient may require dialysis for a few days or weeks until the kidney starts to function.
Did You Know?
The organ most commonly given by a living donor is the kidney. Parts of other organs including the lung, liver and pancreas are also now being transplanted from living donors (source: NKF).
You also can receive a transplant from someone with healthy kidneys willing to donate one to you. The living donor can be a relative, friend, co-worker or someone from your community and can be designated for donation specifically to you. Although the most successful transplants are usually from family members because of a higher likelihood of a better genetic match, there are cases where unrelated donors have been ideal matches. The better the match, usually the lower the chance of rejection. Other advantages of living donor kidneys include the ability to schedule your surgery, usually better kidney quality, increased short- and long-term graft survival, and reduced healthcare cost, according to studies. Also, a kidney from a living donor usually has a higher chance to function immediately upon transplantation, because the kidney is out of the body for a very short time.
For someone to be a living kidney donor, they must be in good physical and mental health. As a general rule, they should be 18 years or older and have normal kidney function. There are some medical conditions that could prevent someone from being a living donor. These include having uncontrolled high blood pressure, diabetes, cancer, HIV, hepatitis or acute infections. Being diagnosed with a serious mental health condition that requires treatment may also prevent someone from being a donor (source: NKF). If you have multiple potential living donors, several can be tested ahead of time to find the best, most compatible donor. The transplant can take place at a time convenient for both the donor and you. (Read more here about how to become a living organ donor.)
How to Get on the Waitlist
Ask your healthcare professional for a referral to a local transplant center or contact a transplant center in your area. Learn as much as possible about the different transplant centers and choose one (or more) that best fits your needs.
Factors you should consider include:
- Insurance coverage and cost
- Location, for going to and from the transplant center both before and after transplant surgery
- If you have a living donor, be sure the transplant center performs living donations; if your live donor is not a good match, check if the transplant center participates in a “paired exchange” program
- Support group availability
Once you choose a transplant center, schedule an evaluation appointment to determine if you are a candidate. Each center has their own criteria for accepting patients. Some may have kidney transplant requirements that include restrictions or rules around age, and also some medical conditions, for example a current or recent cancer diagnosis, may affect the risk of transplant.
Other factors that may affect transplant candidacy:
- Serious heart disease
- General health risk of surviving an operation
- Active infection
- Obesity (being overweight)
- Smoking or substance abuse
If you are a candidate, the transplant team will add you to the national waiting list and will evaluate any potential living donors. While you’re on the waitlist, you will be required to visit your transplant center once a year for tests. These are the same tests you get when you join the waitlist, such as blood tests, urine samples, chest x-rays, blood pressure readings and cancer screenings.
It is possible to list at multiple transplant centers. Often people choose a transplant center closest to their home for convenience, but it is possible to list at multiple transplant centers if you wish (source: NKF). If you have questions about your status on the list, ask the team at your transplant hospital. You will need to let your transplant center know right away if you have changes in your health, your insurance or your contact information.
Did You Know?
The first successful living donor kidney transplant surgery took place in 1954, at what’s now known as Brigham and Women’s Hospital in Boston, MA, by John P. Merrill, M.D. and team, between identical twin brothers (source: Wikipedia).
Average Wait Time
Once you are added to the national transplant waiting list, you may receive an organ fairly quickly, or you may wait many years. In general, the average wait time can be three to five years at most centers, and even longer in some geographical regions of the country. Talk to your healthcare team at your transplant center to get a better understanding of the wait times.
Some factors that determine how long you wait include:
- How well you match with the available kidney
- Your blood group: blood type O has the longest wait, because blood type O donors can donate to other blood groups, but a patient with blood type O can only receive an organ from a donor with blood type O.
- Prior pregnancies, blood transfusions or past transplants: These increase a substance in your body called antibodies. A higher level of antibodies in your blood can make it more difficult to match with a compatible donor.
- How many donors are available in your local area
What to Expect During and After Surgery
A transplant surgery is a surgical procedure to provide you with a healthy kidney. Your native kidneys are usually not removed unless special circumstances are identified by the surgeon. This simplifies the surgery and reduces the risk to you. During surgery, an incision is made in the lower part of one side of the abdomen, the donor kidney is placed, and blood vessels and the ureter from the donor kidney are connected to vessels in the recipient. Once all connections have been made, the incision is closed, with the surgical procedure taking approximately three to four hours to complete. Your kidney transplant scar will fade with time.
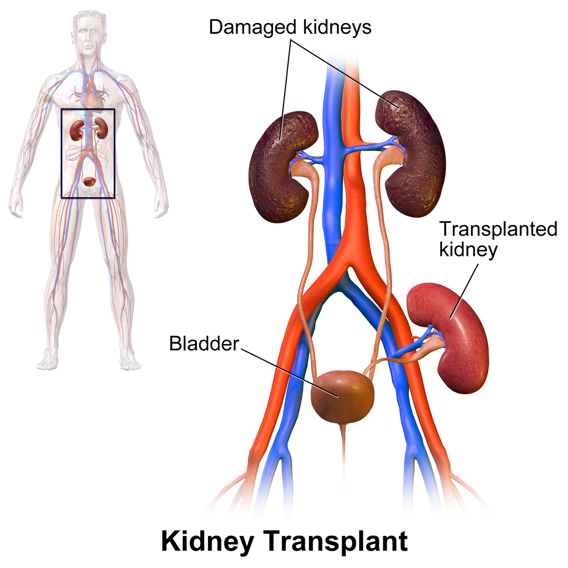
Postoperative care begins with a team of health professionals at your hospital. Comprehensive post-surgical monitoring constantly evaluates whether your body is accepting the new organ. It is important to discuss with your physician what to expect after surgery (source: UNOS).
As with any surgery, complications can occur. These may include:
- Bleeding
- Infection
- Blockage of the blood vessels to the new kidney
- Leakage of urine or blockage of urine in the ureter
- Lack of function of the new kidney at first
Kidney rejection can also occur. Rejection is a result of the normal function of your body’s immune system to a foreign object, tissue or in this case, organ. Without medication to prevent it, when a donor kidney is transplanted into a recipient’s body, the immune system would treat the new organ as a threat and attack or “reject” it. Although rejection is most common in the first six months after surgery, it can occur at any time. Fortunately, a transplant team can usually recognize and treat a rejection episode before it causes any major or irreversible damage.
Because of the risk of rejection, for a transplanted organ to survive, medicines must be taken as prescribed to “quiet” the immune system so it accepts the transplant. These medications are known as “immunosuppressants.” Most immunosuppressant medications are in the form of pills and have some side effects, which will depend on the specific medicines that are prescribed by your doctor. After surgery, it will take your medical team some time to achieve the right balance of immunosuppression for your body. About six months to a year after transplant, immunosuppression is generally lowered and the risk of side effects should be low, according to NKF. It is very important for patients to continuously take their medications as prescribed to avoid rejection and have blood work drawn as scheduled to monitor for any signs that it may be occurring.
Did You Know?
African Americans make up more than one-third of the kidney transplant waiting list nationally, yet only around 13% of the general population. This creates a smaller pool of potential donor organs from African American donors and means that transplant candidates may rely on organs that do not match as well or may have to wait longer for a more suitable match (source: Donor Alliance).
Living with One Kidney
If you receive one transplanted kidney, testing has shown that one organ can work as well as two. Also, the transplanted kidney can increase in size and function (source: NKF).
In the case of living donors, most people live normal, healthy lives with one kidney—also called a solitary kidney. However, it is important for them to stay as healthy as possible. For women who plan to become pregnant after donating a kidney, there are some potential risks related to pregnancy that should be discussed with a doctor prior to donation.
Most people with one healthy kidney do not need to follow a special diet. In general, people with one kidney can keep their organ healthy by staying well hydrated, not taking too much salt, and not gaining excessive weight. Be sure and talk to your doctor about any questions or concerns.
Who Pays for the Cost of a Transplant?
It is important to let your transplant team know what insurance you have, and they can help you determine the costs you may incur both for the transplant surgery and after-care. If you have Medicare coverage, the kidney transplant cost will mostly be covered. If you have a living donor, their costs are usually covered through your insurance as well. Medicare Part B will also cover 80% of the cost of immunosuppressant medications for as long as you have Medicare. (Read more about Medicare coverage for kidney transplant here.)
If you have health insurance from your employer or other private health insurance, most policies cover many costs related to kidney transplants, including medicines. Insurance does not cover other costs like transportation, food and lodging (source: NKF).
How Long Does a Kidney Transplant Last?
Living donor kidney transplant life expectancy is 15-20 years, while deceased donor transplants generally last 10-15 years, according to the American Transplant Foundation.
Kidney transplants are the most successful of all organ transplants, with a 90-95% success rate. According to a recent study, contributions to this success include newer tissue typing and tissue matching platforms, changes in organ allocation systems, living donor paired exchanges, transplant surgical techniques, immunosuppressive medications and patient adherence to their prescriptions, anti-viral medications, refined diagnostic methods of kidney rejection by biopsy, aggressive post-transplant surveillance and overall post-transplant medical management.
Talk to your transplant center staff about their success rates and the national success rates.
What If You Are Not a Candidate?
Unfortunately, transplant is not an option for everyone. You may not be eligible if you have:
- Current or recurring infection that cannot be treated effectively
- Cancer that has spread from its original location to elsewhere in the body
- Severe heart or other health problems that make it unsafe to have surgery
- Serious conditions other than kidney disease that would not get better after transplantation
- Failed to follow the treatment plan
There may be other risks depending on your specific medical condition. Be sure to discuss any concerns with your doctor (source: Johns Hopkins Medicine).
As an alternative to transplant, your doctor may recommend hemodialysis or peritoneal dialysis (PD) at home, or hemodialysis in a clinic.
Outset Medical is passionate about dialysis patients knowing their options and living their best lives. We believe that early kidney disease identification, delay of progression, kidney transplantation and home dialysis are the first-line treatments that all patients should be able to access. Every patient has the option of dialyzing themselves at home, regardless of their personal situation.
The easy-to-learn-and-use TabloTM Hemodialysis System, FDA-cleared for use in the home, hospital or clinic, is revolutionizing how dialysis therapy is delivered. A growing number of patients are taking control of their dialysis and treating on their own schedule at home. Many experts agree that home hemodialysis is the best option (second to transplantation) for treating kidney failure whenever possible, as it can mean greater scheduling flexibility, fewer food restrictions, and better outcomes. Studies have shown that with self-care or home dialysis, many patients actually do better, including fewer hospital visits, better quality of life, longer life expectancy and the ability to maintain employment (visit this page for more information).
Studies also show that home hemodialysis performed more frequently has been associated with similar survival rates as transplantation in the initial five years of therapy, providing an opportunity to serve as a bridge to transplantation, when preemptive and living donor transplantation is not an immediately available option.
Whichever option you choose for dialysis therapy, either while you wait for a kidney transplant or if you are not a candidate for transplant, we encourage you to discuss your wellness goals and all the questions you have with your medical care team.
* Disclaimer:
The information, including but not limited to, text, graphics, images and other material contained on this website are for informational purposes only. No material on this site is intended to be a substitute for professional medical advice, diagnosis or treatment. Always seek the advice of your physician or other qualified healthcare provider with any questions you may have regarding a medical condition or treatment and before undertaking a new healthcare regimen, and never disregard professional medical advice or delay in seeking it because of something you have read on this website.
Tablo Hemodialysis System Disclaimer: Results may vary. Keep in mind that all treatment and outcome results are specific to the individual patient. Please consult your physician for a complete list of indications, warnings, precautions, adverse events, clinical results, and other important medical information. It is important that you discuss the potential risks, complications, and benefits of this product with your doctor prior to receiving treatment, and that you rely on your physician’s judgment. Only your doctor can determine whether you are a suitable candidate for this treatment.
(Source for image at the top of this page: Photo by Abraham Popocatl on Unsplash)